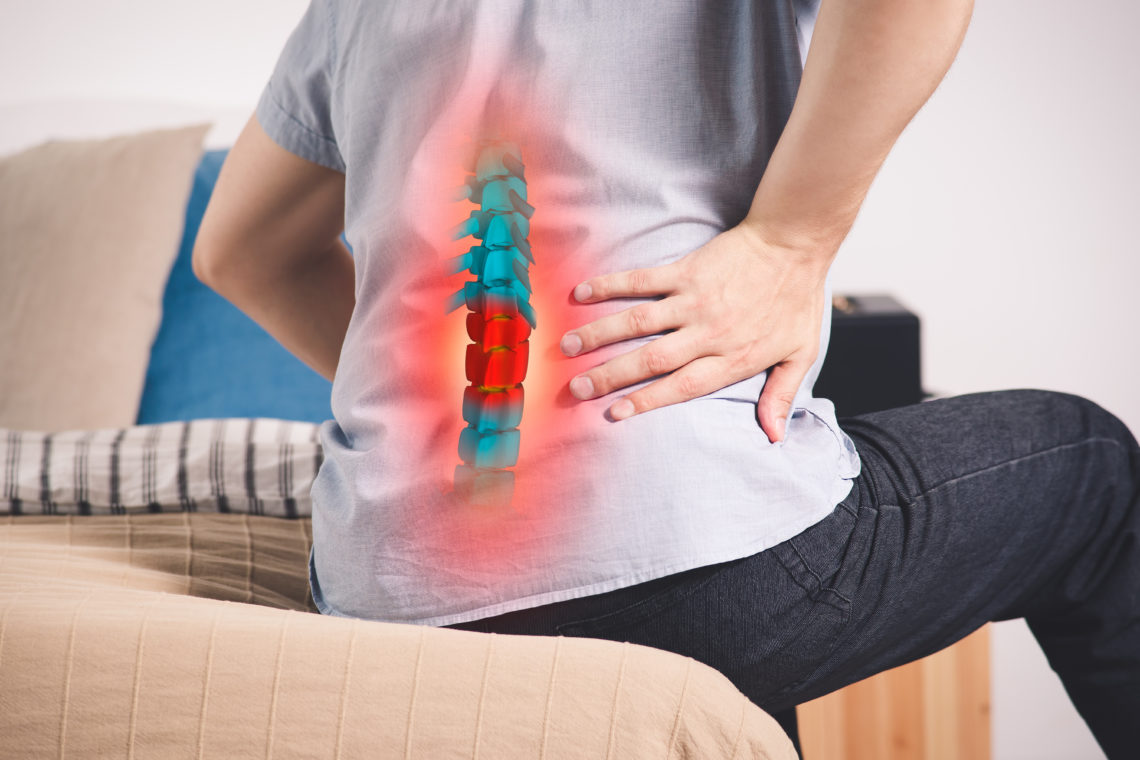
The spinal column extends from the neck to the tailbone. It is comprised of individual vertebrae separated by intervertebral discs. The spinal cord travels behind these discs and gives spinal nerves on each side.
A herniated disc usually results when the soft, gel-like material inside a spinal disc pushes through a tear in its surrounding outer ring of cartilage and can cause pressure on the spinal cord or emerging spinal nerves.
What Are the Symptoms of a Herniated Disc?
A herniated disc can be extremely painful and may cause tingling, numbness, and weakness in the upper and lower extremities and along the body axis depending on its location. For example, pressure from a herniated disc in the cervical spine or neck area may result in pain, numbness, tingling, and weakness in the upper extremities. Similarly, such conditions in the lower lumbar spine can result in symptoms that are noticed in the lower extremities. When this happens in the thoracic spine area, patients may experience pain that radiates along their chest or upper abdomen.
In addition, people may experience pain that worsens with prolonged standing or walking along with stiffness in the affected area. In severe cases, there may be loss of bladder or bowel control, if the compression is along that segment of the spinal cord or the emerging nerves.
A herniated disc may result from overuse or strenuous physical activity, especially in younger people. This can happen after twisting the body towards one side forcefully or after heavy impact like in motor vehicle accidents. In older generations, the basic cause may be degenerative disc disease. Sometimes, the disc may herniate when you turn your body in a specific direction too forcefully. This can also happen with motor vehicle accidents.
Herniated discs are more common in people who do heavy lifting regularly or participate in activities that stress their spines, such as racquet sports and football.
What Can I Do if I Have a Herniated Disc?
If you develop the symptoms of a herniated disc, you should see your doctor immediately. Your physician will perform an examination and may order an X-ray or MRI to determine whether you have a herniated disc.
Many herniated discs symptoms may improve with time and over-the-counter pain medications such as ibuprofen and acetaminophen.
Applying ice packs to your back can help ease the soreness and swelling associated with a herniated disc, too. If these conservative treatment options fail to provide relief or if there is significant pressure placed on the emerging nerve of the spinal cord by the herniated disc, prescription medications and interventional, minimally invasive procedures like epidural steroid injections may be needed. If these fail, surgery may be recommended.
How are Herniated Discs Repaired?
Because the gel-like material inside a spinal disc is surrounded by tissue that helps protect it, surgery is not always necessary to repair a herniated disc. Many people recover from a herniated disc with rest, pain medication, and physical therapy.
However, herniated discs continue to cause severe pain and pressure on the emerging nerves that can require surgery.
For herniated discs, the surgery would usually involve a discectomy. During a discectomy, your surgeon will remove the material from your herniated disc that is pressing against a nerve or causing other problems in your body.
After surgery, patients may feel pain around the incision sites for about eight weeks while the wounds heal. Your doctor may recommend that you wear a brace or cast to immobilize your lower back or neck after surgery.
Final Thoughts
A herniated disc is a common injury. If you believe you have a herniated disc or are experiencing extreme back pain, numbness or weakness, it is best to consult your physician immediately to explore options and avoid long-term consequences. Early management affords the best chance of optimum recovery.